Normal sleep
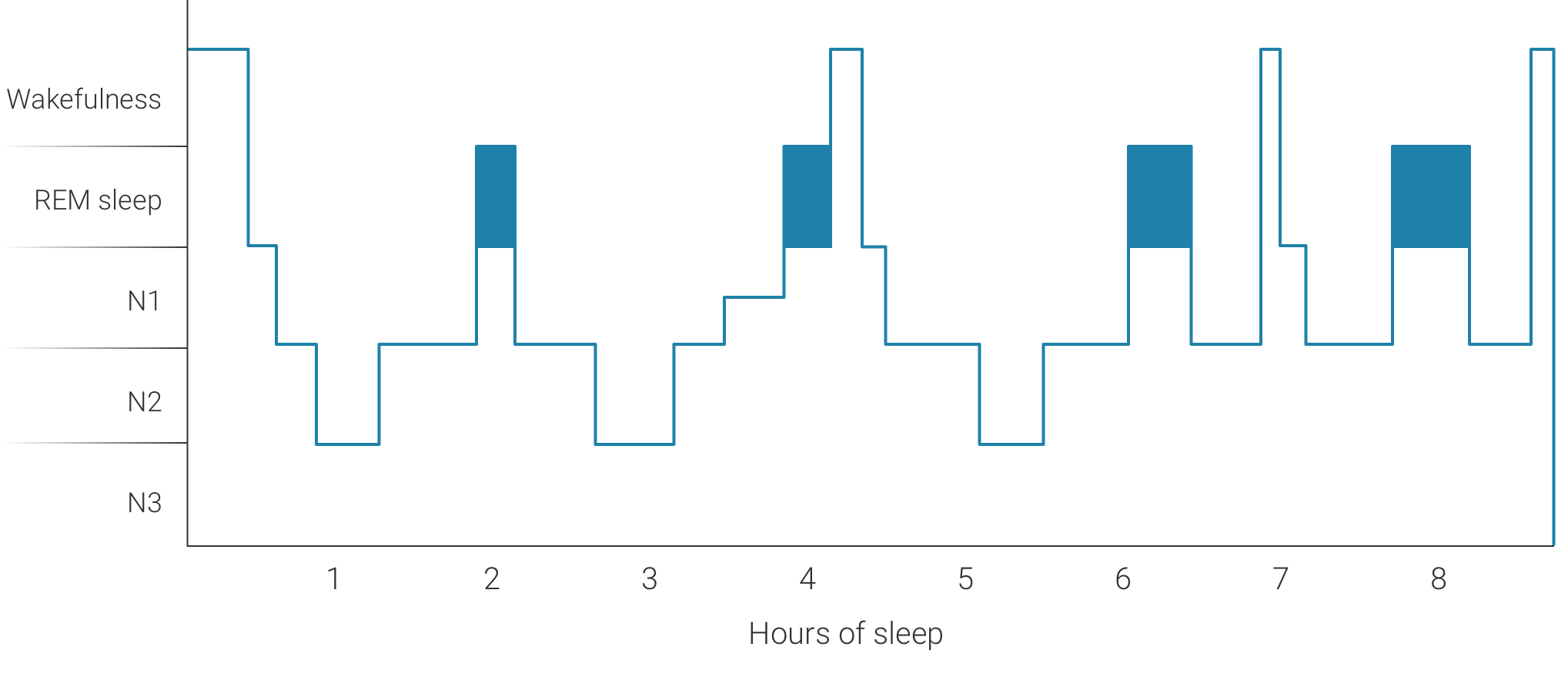
In humans, a normal night of sleep is usually characterized by a succession of stages of slow sleep (or non-REM sleep for non-rapid eye movement) and REM sleep (REM for rapid eye movement). These REM and non-REM sleep stages are usually repeated 4 to 6 times during the night. During non-REM sleep, we distinguish three stages: N1 (light sleep), N2 (slow sleep) and N3 (slow deep sleep). They are named according to certain physiological characteristics including variations of the frequency and the amplitude of brain waves recorded with electroencephalography (EEG). REM sleep, on the other hand, is characterized by the appearance of brain activity similar to what is observed during wakefulness; it is often referred as paradoxical sleep for that reason. It is also during REM sleep that we experience muscle atonia (paralysis of the muscles) as well as rapid eye movements. Dreams are often most intense and detailed during REM sleep.
Many differences are observed between individuals with normal sleep. For example, the number of hours it takes for each person to recover and feel rested the next day varies greatly. However, experts recommend getting 7-9 hours of sleep per night on a regular basis. Sleep also changes with age. In fact, the need for sleep is much greater in children and adolescents, while in the elderly, the sleep episode may be shorter, more fragmented and lighter.
During sleep, there are not only significant changes in brain activity, but also changes in muscle activity, hormonal secretion, autonomic nervous system activity, body temperature, and a multitude of metabolic, cellular, and molecular changes.
Sleep disorders
At least 25% of the population suffers from a sleep disorder requiring the intervention of a healthcare professional. Having poor sleep not only produces discomfort at night but can affect quality of life during the day (e.g., being more irritable, having problems concentrating, being drowsy, being afraid to sleep).
Fortunately, most sleep disorders can be attenuated or sometimes even eliminated with a proper diagnosis and treatment by sleep specialists.
Insomnia
Insomnia is a sleep disorder characterized by a set of symptoms related to a decrease in sleep duration that occurs more than 3 nights per week. Initial insomnia is characterized by difficulty falling asleep; people with this type of insomnia have a very long sleep latency. Very early awakening in the morning is called terminal insomnia. Maintenance insomnia is a difficulty in maintaining sleep and is therefore characterized by numerous and / or prolonged awakenings during the night. Some people with paradoxical insomnia have the impression that they get little or no sleep all night, even though their sleep duration is normal when measured in the laboratory. Their brains may stay more active during sleep, making it seem like they are not sleeping. Sometimes a combination of different types of insomnia can be found in one person. Insomnia of all kinds have adverse daytime consequences such as fatigue and drowsiness, changes in mood and irritability, disturbances in attention and concentration and impaired psychomotor performance.
The diagnosis of insomnia is made when these sleep symptoms interfere with a person's functioning during the day (e.g., difficulty concentrating, irritability, etc.). It is therefore not only the short duration of sleep that is important for the diagnosis, but also the consequences of poor sleep on daytime well-being. Cognitive behavioural therapy is particularly effective in improving insomnia. It helps restore healthy sleep-related behaviours, such as respecting consistent sleep and wake times, and thereby helps a patient to better appreciate the hours they spend in bed.
Hypersomnia
Hypersomnia refers to sleep disorders that are characterized by excessive daytime drowsiness despite having sufficient sleep during the night. The disorders usually start in teenagers or young adults. Patients with hypersomnia have bouts of sleep during the day, unwittingly long naps (sometimes over an hour) which are usually not restorative. These patients experience sleepiness, are difficult to wake up, and waking up is associated with confusion. Idiopathic hypersomnia (without a known cause) is distinguished from secondary hypersomnia which is associated with a physiological problem such as restless legs syndrome or sleep apnea.
Narcolepsy
Narcolepsy is a disorder characterized by sudden bouts of sleep during the day. Patients may experience cataplexy as well as, in some cases, sleep paralysis and hypnagogic hallucinations. Cataplexy is defined by a loss of muscle tone without alteration of consciousness and is triggered by strong emotions such as anger, joy, laughter, or fear. Narcolepsy is distinguished from idiopathic hypersomnia by the restorative effect of naps, sudden bouts of short-lived sleep and falling asleep directly into REM sleep.
REM sleep behavior disorder (RBD)
REM sleep behavior disorder appears mainly after the age of 50 and is clinically characterized by complex and often violent motor behaviors (kicking, punching, fleeing) during sleep. In these patients, there is a loss of muscle atonia, which usually prevents any movement during normal REM sleep. REM sleep behaviors can result in injury to the patient or his/her bed partner. Several longitudinal studies, including those by Drs. Montplaisir, Gagnon and Postuma, have shown that patients with idiopathic REM sleep disorder (no known cause) can develop Parkinson's disease or other dementias such as Lewy body dementia within 10 years of being diagnosed with this sleep disorder.
Somnambulism
Although significantly more common in children, sleepwalking affects 2% to 4% of adults. It usually occurs during the first third of the night, when sleep is deeper. The behaviours that occur during an episode vary from simple actions, such as sitting up in bed or pointing at an object, to very complex activities such as cooking, playing a musical instrument or, rarely, driving a car. Typically, the sleepwalker has open eyes and can interact more or less consistently with other people in the room. Sleepwalkers exhibit disturbed judgment and an altered state of consciousness as well as an erroneous perception of the environment, which can lead to amusing or sometimes dangerous situations. Contrary to popular belief, it is not dangerous to awaken a sleepwalker during an episode. However, it is always best to advise the sleepwalker gently to get back to bed, as waking up suddenly during an episode may lead to confusion or restlessness.
Sleep Apnea
More than 20% of middle-aged adults and almost 50% of people over 65 have symptoms of sleep apnea. We speak of sleep apnea when a person stops breathing for at least 10 seconds and does this repeatedly throughout the night. Most sleep apneas occur when the airways are blocked. This condition causes short but frequent awakenings during the night resulting in a decrease in sleep quality. This leads to daytime sleepiness, headaches and dry mouth upon awakening, and changes in mood and irritability. In the long term, patients suffering from this problem experience cognitive deficits of different types: impairments in general intellectual functioning, attention, alertness, memory, executive functions and manual dexterity. Such patients are also at risk of developing cardiovascular complications. Effective treatments are offered through continuous positive airway pressure (CPAP) devices, dentures, surgery, and weight loss.
Restless Legs Syndrome
Is Restless Leg Syndrome partly genetic? In Quebec, a high percentage of the population has this disorder, and it is in part due to our genes! Restless Leg Syndrome is a disorder characterized by an overwhelming urge to move the lower, and sometimes upper, limbs associated with paresthesias, motor restlessness, increased symptoms at rest with relief from activity, and an increase in symptoms in the evening and/or during the night. This disorder causes difficulty falling asleep as well as frequent awakenings during the night. Walking generally helps to reduce discomfort momentarily. If the symptoms are severe, pharmacological treatment can be used to reduce symptoms and allow better sleep.
Periodic Leg Movement during Sleep (PLMS)
PLMS syndrome is characterized by the repeated, rhythmic onset (often every 20 to 40 seconds) of short duration leg movements during sleep. The most common sleep complaints in patients with PLMS consist of non-restful sleep and daytime sleepiness since these periodic movements cause short arousals that reduce the depth and quality of sleep.
Circadian Disorders
An internal biological clock located in the center of the brain manages all of our physiological behaviours and activities on a 24-hour schedule. This is the case, of course, with our sleep-wake cycle. The internal clock is greatly influenced by the light that reaches our eyes, which is why people who are blind are more at risk of developing a biological rhythm disorder. This group of sleep disorders refers to misalignments of the light-dark cycle that can be either of environmental origin (irregular hours, rotating work, jet lag) or of internal origin (clock dysfunction. biological, blindness, special neurological condition). People with 24-hour arrhythmia have difficulty sleeping at night and staying awake during the day. Circadian disorders include advanced sleep phase syndrome, delayed sleep phase syndrome, irregular sleep-wake rhythm, non-24-hour sleep-wake syndrome, and shift work disorder.

